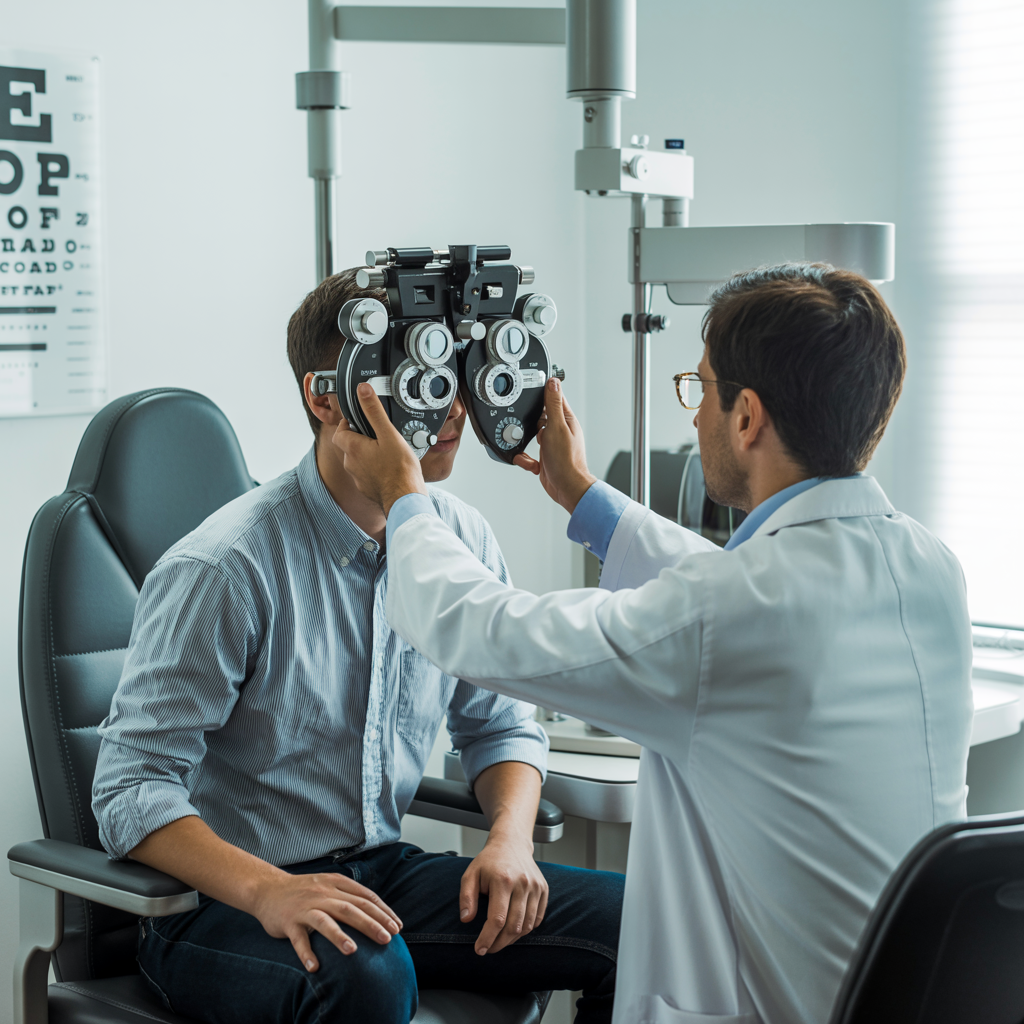
What Type of Lens Does Medicare Cover for Cataract Surgery?
Does Medicare Cover Cataract Surgery?
Medicare covers cataract surgery and includes a standard monofocal intraocular lens (IOL) as part of the procedure. If you’re wondering what type of lens Medicare covers for cataract surgery, after meeting your Part B deductible, Medicare pays 80% of the approved cost, including the surgeon’s fee, facility fee, and the standard lens. However, Medicare does not cover premium lens upgrades such as toric, multifocal, or extended depth of focus (EDOF) lenses. Those upgraded lenses carry an additional out-of-pocket cost that neither Medicare nor most Medigap plans will cover.
Cataracts develop when the eye’s natural lens becomes cloudy over time, causing blurred vision, glare sensitivity, and difficulty seeing at night. Surgery to remove the cloudy lens and replace it with an artificial one called an intraocular lens (IOL) is considered medically necessary when the condition significantly impacts your daily life.
That said, many beneficiaries are surprised to discover that Medicare does not cover all types of lenses. Understanding the difference between what’s covered and what’s considered an upgrade can save you from an unexpected bill — and help you make a more informed decision about your eye care.
How Medicare Covers Cataract Surgery
What Medicare Part B Covers
Cataract surgery is covered under Medicare Part B as a medically necessary outpatient procedure. Part B covers:
- The surgical procedure to remove the cataract
- The surgeon’s fees
- Pre-operative and post-operative eye exams related to the surgery
- One pair of eyeglasses or contact lenses after surgery
- The standard intraocular lens (IOL) is implanted during surgery
After meeting your Part B deductible ($257 in 2026), Medicare Part B typically pays 80% of the Medicare-approved amount. You are responsible for the remaining 20% coinsurance, unless you have a Medicare Supplement (Medigap) or Medicare Advantage plan that covers that portion.
The Standard IOL: What Medicare Pays For
When Medicare approves cataract surgery, it covers the implantation of a monofocal intraocular lens — the standard lens that Medicare has approved as medically necessary.
What Is a Monofocal IOL?
A monofocal lens is designed to correct vision at one focal point — typically either near, intermediate, or far distance. Most patients choose a monofocal lens set for distance vision and then wear glasses for reading or close-up tasks afterward.
Medicare covers the monofocal IOL in full (subject to your Part B deductible and 20% coinsurance). Key features include:
- Corrects vision at a single focal distance (usually distance)
- Does not correct astigmatism
- Does not provide multifocal or near-vision correction
- Covered by Medicare as part of the standard cataract procedure
- Most patients still need reading glasses after surgery
Premium Lenses: What Medicare Does NOT Cover
Surgeons frequently offer premium IOLs that provide enhanced vision correction — but Medicare considers these upgrades beyond what is medically necessary and does not cover the additional cost.
Types of Premium Lenses Not Fully Covered by Medicare
1. Toric IOLs (for Astigmatism)
A toric lens is designed to correct astigmatism in addition to cataracts. Medicare covers the base cost of the cataract surgery, but the extra cost of the toric lens itself is considered a premium upgrade and is billed to you separately.
2. Multifocal IOLs
Multifocal lenses correct vision at multiple distances — near, intermediate, and far — reducing or eliminating the need for glasses. Medicare does not cover the additional cost. These lenses can cost $1,500 to $3,000+ per eye out of pocket.
3. Extended Depth of Focus (EDOF) IOLs
EDOF lenses provide a continuous range of vision, particularly for intermediate and distance tasks. Not covered by Medicare beyond the standard IOL allowance — patients pay the upgrade cost out of pocket.
4. Light Adjustable Lenses (LAL)
Light Adjustable Lenses can be fine-tuned after surgery using UV light treatments, allowing the surgeon to optimize your prescription based on how the eye healed. Medicare does not cover the premium cost above the standard IOL rate.
How the “Upgrade” Billing Works
When your surgeon offers a premium lens, they are required to give you a written notice — called an Advance Beneficiary Notice (ABN) — explaining that Medicare will not cover the additional cost. Here’s how billing works:
- Medicare pays its portion for the surgery, surgeon fees, anesthesia, and the standard IOL.
- You pay your standard cost-sharing — the 20% coinsurance (or your Medigap/Advantage plan pays it).
- The premium lens upgrade cost is billed directly to you as a separate, non-covered charge.
- Neither Medicare nor most Medigap plans cover the premium lens difference.
Important: Medicare Supplement (Medigap) plans only cover Medicare-approved charges. Since the premium lens upgrade is not Medicare-approved, Medigap does not cover that portion either.
Laser-Assisted Cataract Surgery: Is It Covered?
Laser-assisted cataract surgery uses a laser to make incisions and soften the cataract before removal. Medicare considers this a premium upgrade to the standard manual procedure:
- Medicare covers the standard manual cataract surgery (subject to cost-sharing)
- The additional cost of the laser is billed to the patient as a non-covered charge
- Typical out-of-pocket costs range from $500 to $1,500 per eye
Does Medicare Advantage Cover Cataract Surgery?
If you’re enrolled in a Medicare Advantage (Part C) plan, cataract surgery coverage follows the same basic rules as Original Medicare — but your cost-sharing may differ.
- The surgery itself is covered under your plan’s medical benefits
- Your copay or coinsurance depends on your specific plan
- Premium lenses are still generally not covered
- Some plans include additional vision benefits that may partially reimburse eyewear after surgery
- Always verify in-network surgeons and facilities before scheduling
Tip: If you have a Medicare Advantage plan, call member services or contact your broker to verify coverage details before your surgery date.
The Post-Surgery Eyeglasses Benefit
After cataract surgery, Medicare does cover one pair of conventional eyeglasses or contact lenses — one of the very few times Medicare covers corrective eyewear.
- One pair of glasses or one set of contact lenses per eye operated on
- Must be purchased from a Medicare-enrolled supplier
- Standard frames and lenses are covered (subject to 20% coinsurance after deductible)
- Upgrades to premium frames or progressive lenses may carry additional out-of-pocket costs
Medicare Cataract Lens Coverage at a Glance
| Lens Type | Medicare Covers? | Patient Responsibility |
|---|---|---|
| Standard Monofocal IOL | ✅ Yes (80% after deductible) | 20% coinsurance |
| Toric IOL (astigmatism correction) | ⚠️ Partially | Premium lens upgrade cost |
| Multifocal IOL | ⚠️ Partially | Premium lens upgrade cost |
| EDOF IOL (e.g., Symfony) | ⚠️ Partially | Premium lens upgrade cost |
| Light Adjustable Lens (LAL) | ⚠️ Partially | Premium lens upgrade cost |
| Laser-Assisted Surgery (add-on) | ❌ No | Full laser upgrade cost |
| Post-Surgery Eyeglasses (standard) | ✅ Yes (80% after deductible) | 20% coinsurance |
Questions to Ask Your Surgeon Before Surgery
- What type of IOL do you recommend for my specific vision needs?
- Is the lens you’re recommending covered by Medicare, or is it a premium upgrade?
- What will I owe out of pocket for the lens, the facility, and the surgeon?
- Will I still need glasses after the procedure?
- Do you accept Medicare assignment?
Frequently Asked Questions
Yes. Medicare covers cataract surgery on each eye separately as a medically necessary procedure. Each surgery is billed individually.
Yes. The out-of-pocket cost for premium IOL upgrades is generally an eligible expense for Health Savings Accounts (HSA) and Flexible Spending Accounts (FSA). Consult your plan administrator for specifics.
If your surgeon does not accept Medicare assignment, they may charge up to 15% more than the Medicare-approved amount. This excess is billed directly to you.
Prescription eye drops are generally covered under Medicare Part D (prescription drug coverage), not Part B. Coverage depends on your specific Part D formulary.
Yes. If you are enrolled in a Medicare Savings Program (such as QMB), your Medicaid program may cover some or all of your Medicare cost-sharing for the surgery.
Need Help Understanding Your Medicare Benefits Before Surgery?
Navigating Medicare coverage can feel overwhelming. At Craig Smith Insurance Group, I work with Medicare beneficiaries across Queens, Long Island, Westchester, the Bronx, and New Jersey to help them understand their benefits at no cost to you.
Medicare coverage rules are subject to change. This article is for informational purposes only and does not constitute legal, medical, or financial advice. Craig Smith