Types of Dental Plans
Dental Insurance in Layman’s Terms. two main types of dental plans are DMOs, or Dental Maintenance Organizations, and Passive PPOs. A DMO is sort of like an HMO. Typically, you must choose a dentist from the plan’s provider network and then get referrals if you need to see a specialist. Payment for most covered services under the plan are based on a fee schedule. What this means is that, for a given procedure, the member is charged a flat dollar amount. That can be good because the member knows ahead of time what the charge is. It can be bad because many established dentists choose not to participate in DMO networks due to the lower reimbursement rates.
The other type of dental plan, which provides more freedom to see whatever dentist you’d like, is a passive PPO. Under these plans, the provider network is larger, and the member does not have to choose a primary dentist. Even more importantly, the member can visit a dentist outside of the network and still receive reimbursement for the services. For the remainder of this article, we’ll focus on passive PPO plans.
Plan Deductible
Like most health plans, a dental PPO plan will have a calendar-year deductible, but instead of the $5,000 to $8,000 deductibles that are common for health insurance policies, the deductible on a dental plan is often in the $25-50 range. It can be higher, but most deductibles are quite reasonable. There will also be a family deductible if multiple people are covered under the dental plan. It is usually two or three times the individual deductible amount.
Three Levels of Coinsurance
Also like most health plans, the member pays a coinsurance amount after the calendar-year deductible has been met. What’s different is that the coinsurance percentage will vary depending on the type of service. On most dental PPO plans, there are three levels of coinsurance: one for preventive care, one for basic services, and one for major services. The most common coinsurance levels are 100-80-50. What this means is that, after the deductible has been met, the plan pays 100% of the cost for preventive care, 80% of the cost for basic services, and 50% of the cost for major services. The member is responsible for the remaining amount.
Of course, it’s important to read the policy to determine how the services are classified. For instance, periodontics and endodontics might be covered as a major service, meaning that the policy would pay 50% of the cost in our example, or they could be covered as a basic service, meaning that the policy would pay 80% of the cost. The more services that are covered as a basic benefit, the better the plan, but it will also be more expensive. It’s also important to note how often preventive care will be covered. For instance, many policies will allow for two cleanings per year, but the member might have to wait six months between cleanings.
Annual Maximum
Where a dental plan really differs from a medical plan is that health insurance policies have an out-of-pocket maximum—the most the member might have to pay in a given year. That’s not how dental insurance works. Instead, dental plans have an annual maximum benefit—the most the plan will pay per year. So, if a plan has a $1,000 annual maximum, that means that, in addition to any network discounts the member enjoys, the insurance plan will pay up to $1,000 of dental expenses after the calendar-year deductible has been satisfied. Usually, anything the plan pays, whether for preventive services, basic service, or major services, counts toward the annual maximum, but it’s important to double-check. Some plans may not apply the cost of preventive care to the annual limit, which of course is an enhancement to the policy.
Typically, annual maximums on a dental plan are in the $750 to $3,000 range, though that can vary. The higher the annual maximum, the better the policy, but the more expensive it will be.
Waiting Period
Many dental plans, especially those sold in the individual market, have a 12-month waiting period for major services if the member does not have prior dental coverage. This is very important to mention to the client. Often, people wait until they need medical or dental care to begin shopping for insurance, so they need to understand that they might need to have the policy for a full year before the more costly major services will be covered. It is possible, depending on the plan, that the member will benefit from the network discounts on major services even before the waiting period is satisfied.
Out-of-Network Coverage
Perhaps the biggest difference between health and dental coverage is in the way out-of-network services are covered. On a health plan, when the member goes out of network, not only is there no discount since the providers are not contracted, there is also a higher deductible and higher coinsurance amount—usually twice the in-network amount. Additionally, most health plans pay the same discounted amount for out-of-network services that they would have paid to contracted in-network providers, which means that the non-network provider is very likely to balance bill the member.
That is not the way dental insurance works. Under most passive PPO dental plans, there is not a separate calendar-year deductible for non-network services, and the coinsurance levels are not reduced when receiving care outside the contracted provider network. In other words, on a 100-80-50 plan, the policy will still pay 100% of the allowed amount for preventive services, 80% of the allowed amount for basic services, and 50% of the allowed amount for major services when they are received from a non-network dentist.
Where dental plans differ from one another is in how they determine the allowed amount. Some plans, similar to the way health insurance works, will pay the same discounted amount out of network as they would pay a contracted in-network dentist. This is known as a Maximum Allowable Fee (MAF) or Maximum Allowable Charge (MAC) arrangement, and because non-network dentists have not agreed to a discounted rate for the services they provide, they are likely to balance bill the member for any amount not covered by the dental plan.
Other plans pay the applicable coinsurance percentage (depending on whether it’s a preventive, basic, or major service) of a higher allowed amount. This amount is determined by what most dentists in the area would charge for the given procedure. These plans might pay based on 80% or 90% of the “reasonable and customary” (R&C) or “usual and customary” (U&C) amount. What this basically means is that the allowed amount is set at a level where eight out of 10 or nine out of 10 dentists in the area would accept this allowed amount as their total payment. The other 10 to 20 percent of dentists are likely to balance bill the member. Long story short, an R&C plan will pay non-network dentists a higher amount than an MAF plan, making it less likely that the member will be billed an amount above their applicable coinsurance.
Orthodontics
Another way that dental plans differ from one another is in their coverage of orthodontics. Some plans do not cover ortho at all; others might offer a discount but no payment; others will cover child orthodontics up to an annual and lifetime maximum, and still, others will cover adult orthodontics up to an annual and lifetime maximum. The annual limit for orthodontics is usually separate from the annual limit for other covered services.
Limitations & Exclusions
As with health coverage, it’s always important to review the limitations and exclusions on a dental plan. While some services will be excluded from most dental plans, there may be some differences, so this is worth reading. One example of an item that will be covered on some dental plans but excluded on others is dental implants.
Only a Summary
Please remember that this is only a summary of how dental insurance works, and there may be additional differences between one plan and another, but hopefully, this article gives you some ideas about how to explain dental coverage to your clients. Dental insurance is important, especially when we consider how many medical conditions can be detected during a dental visit and how poor dental care can cause or worsen other medical conditions.
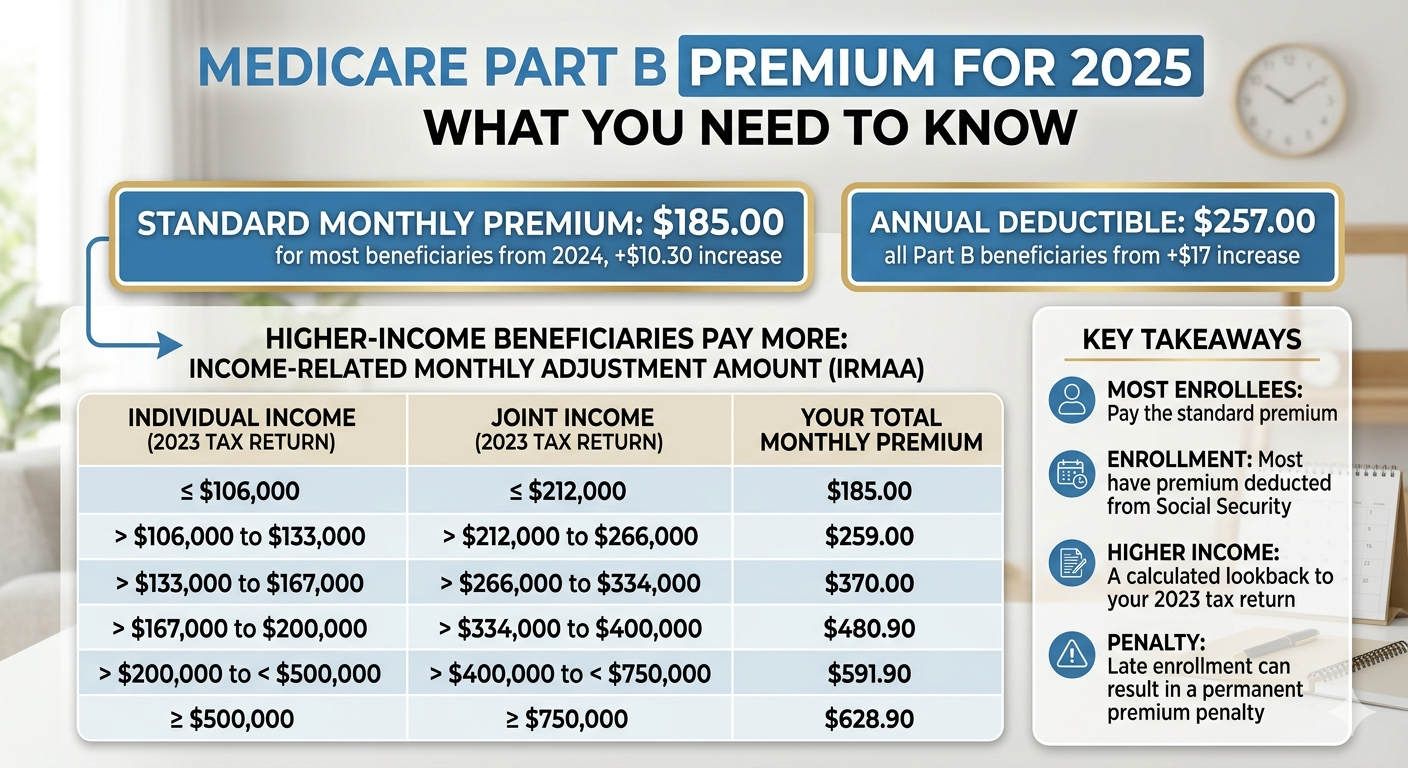
Does Medicare Cover Dental?
Review our post on Dental Coverage Under Medicare and Dental Insurance

Craig Smith
Independent Medicare Insurance Broker | AHIP Certified
Craig Smith is the founder of Craig Smith Insurance Group, an independent Medicare brokerage serving seniors across New York, New Jersey, and nationwide since 2013. With over 25 years of financial services experience and 149+ five-star Google reviews, Craig helps clients compare Medicare Advantage, Medicare Supplement, and Part D plans — always free of charge.
Learn more about Craig →